Short Term Disability Claims Preparation
Automate both Standard and Special Handling Claims Preparation processes to reduce manual handling time while improving data quality.
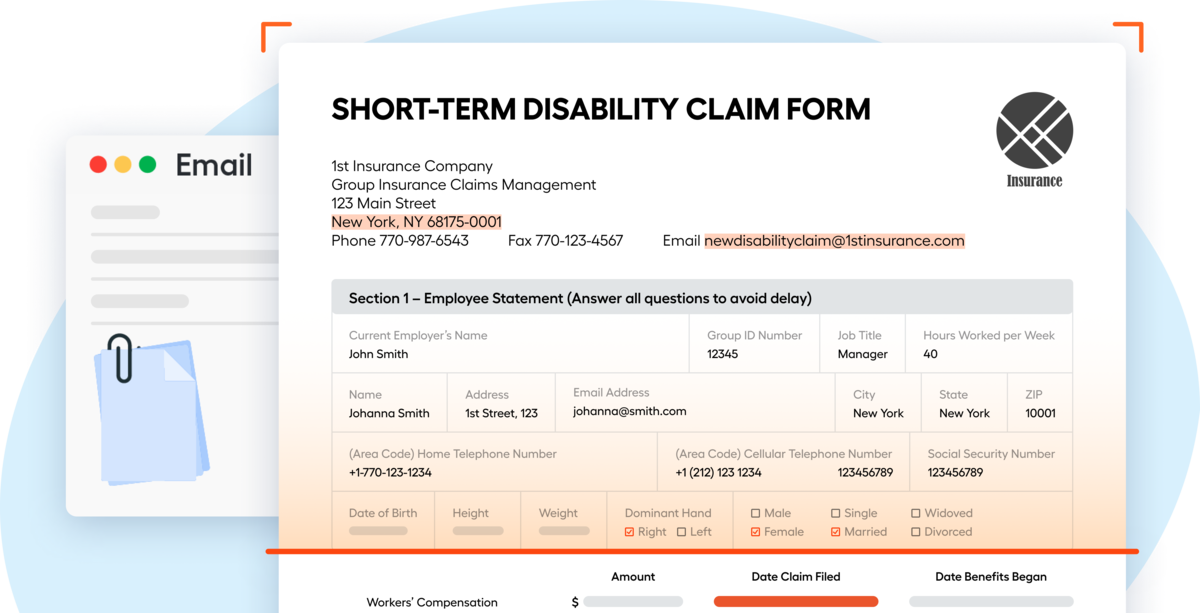
What needs to be changed
Insurers today are under pressure to effectively meet changing consumer expectations, shorten processing times, and efficiently manage claims.
Speed, accuracy, and efficiency (e.g., not asking for the same customer data twice) are paramount to the insurance customer experience.
Moreover, insurers also must compete on cost and optimize for their combined ratio. To that end, it’s important for them to seize every opportunity to reduce manual work in operations.
Challenges
Currently, standard claims preparation and special handling of claims require long manual handling times. Challenges include:
- Intensive manual work: Ops personnel select transactions from the claims processing system by hand.
- Multiple systems for claims routing:
- Orchestration tool
- Claims information data entry for multiple systems of record (e.g., for claims data, for billing and eligibility)
- Document repository for intake documents
- Slow turnaround times: Multiple rounds of manual work (due to errors) slow down turnaround times
- High costs: 40+ FTEs perform this manual work
WorkFusion's solution
From day 1, WorkFusion’s pre-built Intelligent Automation solution for Claims Preparation and Claims Processing achieves 80% straight-through processing for Standard Claims Prep and 50%+ reduction in handling time for Special Handling Claims:
- It collects and classifies documents into types via ML models
- Extracts key data points from documents
- Develops data validation rules
- Displays data in WorkSpace task
- Pushes final structured data into core systems and sends notifications for early claims submission
- Gathers additional data from ClaimFacts and Zeus
- Sends notifications and creates reminders/follow-ups
- Optimizes ML models
The solution automates and streamlines work in a large number of applications:
- Workflow tools to orchestrate tasks within Short Term Disability Claims Prep process
- Enterprise Service Management services that integrate with ClaimFacts to generate claim number, which updates into workflow tool
- Document repositories and systems of record for intake documents
- Mainframe-based systems of record for claims data
- Mainframe-based systems of record for billing and eligibility
- Microsoft Exchange Server: Email client for employee outreach
Document types
- Paper claims
- Family and Medical Leave Act (FMLA) claims
Supported integrations
- Microsoft Exchange Server
- ClaimFacts
- Zeus Claim
- TeleGuard
- Guardian Anytime